|
Polyp (medicine) - Wikipedia. For polyps on the skin (skin tags), see Acrochordon. For the small aquatic animal, see Polyp. 
A polyp is an abnormal growth of tissue projecting from a mucous membrane. If it is attached to the surface by a narrow elongated stalk, it is said to be pedunculated. If no stalk is present, it is said to be sessile. Polyps are commonly found in the colon, stomach, nose, ear, sinus(es), urinary bladder, and uterus. They may also occur elsewhere in the body where mucous membranes exist like the cervix. Some polyps are tumors (neoplasms) and others are nonneoplastic (for example, hyperplastic or dysplastic). The neoplastic ones are generally benign, although some can be premalignant and/or concurrent with a malignancy. Digestive polyps. Occasionally rectal bleeding, and on rare occasions pain, diarrhea or constipation may occur because of colon polyps. Colon polyps are a concern because of the potential for colon cancer being present microscopically and the risk of benign colon polyps transforming over time into malignant ones. Since most polyps are asymptomatic, they are usually discovered at the time of colon cancer screening. Common screening methods are occult blood test, colonoscopy, sigmoidoscopy (usually flexible sigmoidoscopy, using a flexible endoscope, but more rarely the older rigid sigmoidoscopy, using a rigid endoscope), lower gastrointestinal series (barium enema), digital rectal examination (DRE), and virtual colonoscopy. Deyhle, Germany, 1. If an adenomatous polyp is found with sigmoidoscopy or if a polyp is found with any other diagnostic modality, the patient must undergo colonoscopy for removal of the polyp(s). Even though colon cancer is usually not found in polyps smaller than 2. When adenomatous polyps are removed, a repeat colonoscopy is usually performed in three to five years. Most colon polyps can be categorized as sporadic. Inherited polyposis syndromes. The adenomatous polyp is considered pre- malignant, i. They are unlikely to develop into colorectal cancer. About 5% of people aged 6. Most polyps (approximately 9. The remaining 1. 0% of adenomas are larger than 1 cm and approach a 1. They tend to be non- pedunculated, velvety, or cauliflower- like in appearance and they are associated with the highest morbidity and mortality rates of all polyps. They can cause hypersecretory syndromes characterized by hypokalemia and profuse mucous discharge and can harbor carcinoma in situ or invasive carcinoma more frequently than other adenomas. The risks of progression to colorectal cancer increases if the polyp is larger than 1 cm and contains a higher percentage of villous component. Also, the shape of the polyps is related to the risk of progression into carcinoma. Polyps that are pedunculated (with a stalk) are usually less dangerous than sessile polyps (flat polyps). Sessile polyps have a shorter pathway for migration of invasive cells from the tumor into submucosal and more distant structures, and they are also more difficult to remove and to ascertain. 
Sessile polyps larger than 2 cm usually contain villous features, have a higher malignant potential, and tend to recur following colonoscopic polypectomy. Larger tubular adenomatous polyps have an increased risk of malignancy when larger because then they develop more villous components and may become sessile. It is estimated that an individual whose parents have been diagnosed with an adenomatous polyp has a 5. Overall, nearly 6% of the population, regardless of the family history, is at risk of developing colon cancer. Screening. Medical societies have established guidelines for colorectal screening in order to prevent adenomatous polyps and to minimize the chances of developing colon cancer. It is believed that some changes in the diet might be helpful in preventing polyps from occurring but there is no other way to prevent the polyps from developing into cancerous growths than by detecting and removing them. According to the guidelines established by the American Cancer Society, individuals who reach the age of 5. Test Overview. Colonoscopy is a test that allows your doctor to look at the inner lining of your large intestine (rectum and colon). He or she uses a thin, flexible. 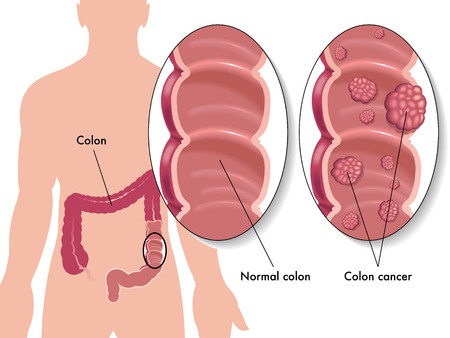
Colon polyps as they grow can sometimes cause bleeding within the intestine, which can be detected with the help of this test. Also, persons in their 5. If adenomatous polyps are detected during this procedure, it is most likely that the patient will have to undergo a colonoscopy. Medical societies recommend colonoscopies every ten years starting at age 5. 
Once an adenomatous polyp is identified during colonoscopy, there are several methods of removal including using a snare or a heating device. While there are risks of complications associated with colonoscopies, those risks are extremely low at approximately 0. For comparison, the lifetime risk of developing colon cancer is around 6 percent. Commonly occurring, they are experienced by up to 1. They are overgrowths of the mucosa that frequently accompany allergicrhinitis. They are freely movable and nontender. 
Laryngeal polyps. They can occur on one or both vocal folds, and appear as swelling, a bump (similar to a nodule), a stalk- like growth, or a blister- like lesion. Most polyps are larger than nodules, which are more similar to callouses on the vocal folds. Polyps and nodules can exhibit similar symptoms including hoarseness or breathiness, “rough” or “scratchy” voice, harshness in vocal quality, shooting pain from ear to ear, sensation of having “a lump in the back of the throat”, neck pain, decreased pitch range in the voice, and vocal and bodily fatigue. If an individual experiences symptoms for more than 2 to 3 weeks, they should see a physician. For a diagnosis, a thorough evaluation of the voice should include a physical examination, preferably by an otolaryngologist (ear, nose, and throat doctor) who specializes in voice, a voice evaluation with a speech- language pathologist (SLP), a neurological examination (in certain cases) The qualities of the voice that will be evaluated include quality, pitch, loudness, and ability to sustain voicing. In some cases, an instrumental examination may be performed with an endoscope into the mouth or nose; this gives a clear look at the vocal folds and larynx in general.  
In addition to this, a stroboscope (flashing light) may be used to observe the movement of the vocal folds during speech. Polyps may be treated with medical, surgical, or behavioral intervention. Surgical intervention involves removing the polyp from the vocal fold. This approach is only used when the growth(s) are very large, or have existed for an extended amount of time. In children, surgical intervention is rare. Existing medical problems may be treated in an effort to reduce the strain and negative impact on the vocal cords. This could include treatment for gastrointestinal reflux disease, allergies, and thyroid problems. Intervention to stop smoking and reduce stress may also be needed. Most people receive behavioral intervention, or vocal therapy, from an SLP. This might involve teaching good vocal hygiene, and reducing or stopping vocal abuse behaviors. Direct voice treatments may be used to alter pitch, loudness, or breathe support to promote good voicing.^Weschler, Toni (2. Taking Charge of Your Fertility (Revised ed.). New York: Harper. Collins. ISBN 0- 0. Endoscopy (Suppl): 3. PMID 7. 40. 87. 89. Retrieved 2. 01. 0- 0. Retrieved 2. 01. 0- 0. Retrieved 2. 01. 0- 0. Retrieved 2. 01. 0- 0.
I am having a colonoscopy and endoscopy tomorrow and was given the preparation of 236 grams of Miralax to be mixed in two 32 oz bottles of Gatorade, 4 Dulcolax. 
Retrieved 2. 01. 0- 0. Gastroenterology. PMID 1. 25. 57. 15. Retrieved 2. 01. 0- 0. 
Retrieved 2. 01. 0- 0. Practical Gynaecological Ultrasound. Cambridge University Press. ISBN 1- 9. 00. 15. Mayo. Clinic. com. Retrieved 2. 00. 7- 1. Mills; Darryl Carter (2. Sternberg's Diagnostic Surgical Pathology. Lippincott Williams & Wilkins. ISBN 0- 7. 81. 7- 4. Merck Manual of Diagnosis and Therapy. Retrieved 2. 00. 7- 1. Suurmeijer (1. 99. The Pap Smear. Taylor & Francis. ISBN 3- 7. 18. 6- 5. Practical Gynaecological Ultrasound. Cambridge University Press. ISBN 9. 78- 1- 9. The Pros and Cons of Colonoscopy. By Dr. Mercola. Colon cancer is the second leading cause of cancer- related deaths in the United States. According to the Centers for Disease Control and Prevention (CDC),1 nearly 1. As reported by Reuters: 4“About 1,0. FOBT or colonoscopy, or given a choice between the two options. Over three years, 4. Just 1. 4 percent of the patients assigned to FOBT got the test done each year.”Side Effects and Drawbacks of Colonoscopies You Need to Be Aware Of. As noted in the video above, narrated by Dr. Michael Greger, about 1 in every 3. Death from colonoscopy, while rare, also does occur. Part of the reason for this is that in other countries doctors do not get paid for procedure referrals. Greger, “it’s estimated that doctors make nearly a million more referrals every year than they would have if they there were not personally profiting.”. Unfortunately, most doctors also fail to inform their patients of the risks of colonoscopy, which include: 6,7. Perforation of the colon (people at higher risk include those with diverticulitis, diseases of the colon, and adhesions from pelvic surgery). Dysbiosis and other gut imbalances, caused by the process of flushing out your intestinal tract before the procedure with harsh laxatives. Complications from the anesthesia. Many experts agree you should opt for the lightest level of sedation possible, or none at all, as full anesthesia increases risks. False positives. According the Prostate Cancer Foundation,9 an estimated 3. Preventive Services Task Force, “you’re going to die with them, not of them.”. False positives lead to unnecessary treatments that are nearly always harmful, in addition to the anxiety a cancer diagnosis brings. For example, incontinence and erectile dysfunction are two common side effects of radiation therapy, and hormone therapy has been linked to osteoporosis and depression. These devices are not disposable, so they must be sterilized between each use. This, it turns out, poses a very significant problem that most patients are not aware of. One is a long, flexible tube with a tiny camera at the end, which allows the doctor to view the inside of your colon. There are also two internal channels in this tube, a biopsy channel and an air/water channel. The air/water channel allows the doctor to clean the lens of the camera, which frequently gets covered with blood and other patient material. So, the problem, in a nutshell, is that doctors are re- using devices that are impossible to properly clean. So if, for whatever reason, you are compelled to get a colonoscopy or flexible sigmoidoscopy, then it is IMPERATIVE that you contact the office before the procedure to make sure they are decontaminating the scope properly with peracetic acid. When Getting a Colonoscopy, Make Sure Peracetic Acid Was Used to Clean the Scope. Lewis launched a study with a university in which he looked at the internal channels, the air/water channel, and the biopsy channel, and collected samples of patient material from those channels. He then tested various ways of treating that layer of patient material to determine what was required to remove it from the inner channels. In fact, Lewis demonstrated that you can submerge those devices for two hours and there’s still infectious material, such as HIV, trapped inside those internal channels. About 2. 0 percent of flexible endoscopes in the U. S. Peracetic acid (which is similar to vinegar) is used in organic chemistry labs to dissolve proteins, and it does a FAR better job than glutaraldehyde. Even pennies per procedure add up when you’re doing them by the thousands each year, and hospitals are under pressure to save money wherever they can. How will you know how any given facility cleans their scopes? You have to ask. If you’re having a colonoscopy or any other procedure using a flexible endoscope done, be sure to ask: How is the endoscope cleaned between patients? Specifically, which cleaning agent is used? How many of your colonoscopy patients have had to be hospitalized due to infections? If the hospital or clinic uses peracetic acid, your likelihood of contracting an infection from a previous patient is very slim. If the answer is glutaraldehyde, or the brand name Cidex (which is what 8. As for the third and last question, the answer you want is zero. Prepping for Your Colonoscopy. Getting a colonoscopy requires preparation to clean out your colon. Typically, this includes skipping dinner and breakfast before the procedure, and drinking 2 to 4 liters of a foul- tasting liquid containing laxatives and electrolytes. However, recent research suggests you may not have to go through the rigors of fasting — a step that dissuades many from getting a colonoscopy in the first place. The patients, aged 4. Eight of the first 1. None reported bloating, nausea, vomiting, or cramping. When they examined the patients, doctors rated 9 of the 1. Greger at Nutrition. Facts. org. 12 presents yet another alternative: peppermint, which helps relax the muscles and reduce spasms in your colon. The use of peppermint during colonoscopy was suggested over three decades ago, but was never implemented. As noted by Dr. Greger in the video above: “. So, they tried spraying some peppermint oil at the tip, and in every case, the spasm was relieved within 3. Thirty seconds is a long time though when you have this snaking inside of you; so, the next innovation would be to just use a hand pump to flood the whole colon with a peppermint oil solution before the colonoscopy. Even taking a few peppermint oil capsules orally, four hours before the procedure, helped speed up the procedure by reducing spasms and pain. Should You Have Routine Colonoscopies Starting at 5. While I believe they can be valuable as a diagnostic tool, I feel confident that with my diet (which includes daily amounts of raw turmeric) and lifestyle it’s highly unlikely I would develop colon cancer. But for many people who are at higher risk, colonoscopies may be an effective strategy. Colon cancer grows very slowly, and it’s one of the top leading cancers that kill people, so early detection is important. Another alternative is to get tested by flexible sigmoidoscopy. It’s similar to a colonoscopy, but uses a shorter and smaller scope, so it cannot see as far up into your colon. On the upside, it’s associated with fewer complications, although you still need to check with the hospital or clinic to make sure they’re using peracetic acid to clean the device. If polyps are found in their early stages, your doctor can simply snip them off right then and there. So a colonoscopy is not only a diagnostic tool, it can also serve as a surgical intervention. They take a picture of the polyp, clip it, capture it, and send it to biopsy. So it could save your life, and it’s definitely something to consider. So please remember, asking what they use to clean the scope could save your life. Only agree to the procedure in a facility that uses peracetic acid as a cleaning solution. This is a very simple strategy that will not only protect your health, but as more people get wise to this and start demanding the use of peracetic acid, we can improve the safety for all patients undergoing these procedures.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
